Keratoconus
Table of Content
Keratoconus is one of the progressive dystrophies of the cornea, caused by inborn metabolic disorders.
It is believed that abnormal collagen cross-link structure of the corneal stroma is the reason, which leads to thinning of the stroma and corneal distension, but peripheral zones are retained. Presumably, changes occur primarily in the basal cell layer of the corneal epithelium. Secretion of proteolytic or autilytic enzymes from damaged corneal epithelial cells may result in depolymerization of sulphide connections in hyaluronic acid, which causes damage to stromal collagen fibers.
Keratoconus usually manifests itself in the second or third decade of life. By definition, that applies to both eyes and the degree of development is usually different. Some cases of unilateral cone are treated as a state of different lesion advancement. The disease is progressive and most frequently changes are progressing by leaps and bounds, after which there may occur differently long lasting periods of stability. Mental crises, hormonal changes, stress may contribute to disease progression. In over 55 –year old patients, development of changes is usually stopped.
The incidence of disease given by different authors , varies from 1:1000 to 1:2500, however , it is clearly increased in the areas of “closed” genetically (e.g . in island countries).
Older studies indicate that incidence in women was more numerous, however, more recent research shows more in men.
Keratoconus is more common in general diseases like Down’s syndrome, Turner, Ehlers-Danlos syndrome, Marfan syndrome in atopic diseases, osteoporosis imperfecta, mitral valve prolapse and ocular disorders such as vernal keratoconjunctivitis, anirydia, Leber’s congenital blindness, pigmentary degeneratiion of retina , ectopia lentis.
Symptoms of keratoconus:
- rapid progressive deterioration of visual acuity
- rapid progressive blurring, distortion of the image in one eye
- rapidly growing astigmatism and myopia in one eye
- blurring of the image (poliopia monocular)
- sensitivity to light (photophobia)
- itching and redness in eyes
- symptom of a halo around the light source (blurred sharpness of vision)
- rarely, the first symptom is so-called sharp cone – a sudden hazy vision, which may persist for several weeks and cause eye pain
Munson symptom is one of the subjective symptoms.
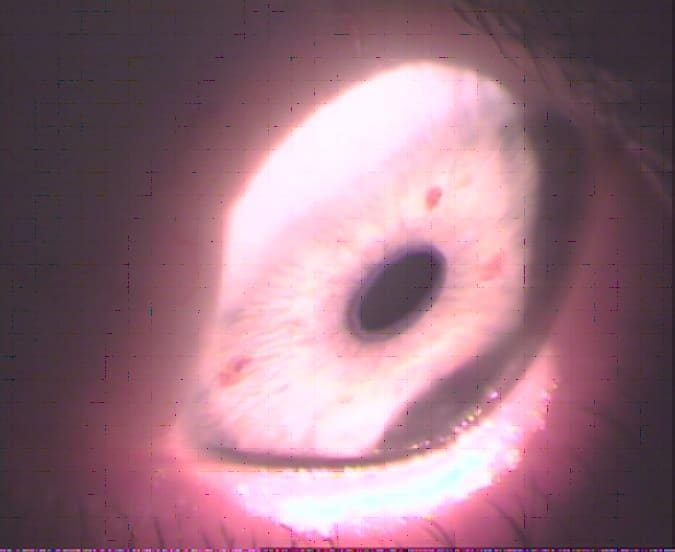
Photo. 1. Munson`s symptom

Fig.1 Example of corneal topography with a cone located far on the circuit. In this examination, we diagnosed astigmatism and small Amsler angle in ophthalmometer test of central waves.

Photo. 2. Turbidity caused by rupture of Descemat membrane.

Photo. 3. Supra -membrane turbidity caused probably by sub epithelial chronic erosion of the cornea.

Photo. 4. Supra-membrane turbidity caused probably by sub epithelial chronic erosion of the cornea.
Classification of keratoconus
Classification by Amsler – expanded by Dieter Muckenhirna by the cornea cam.
| Degree | Amsler’s angle | Mid rays | Acuity
glasses |
Acuity
contact lenses |
Transparency | Cornea
thickness |
Can |
|---|---|---|---|---|---|---|---|
| 1 | 0-3 | >7.5 | 1.0-0.8 | >1 | Normalna | 0.5 | <0.8 |
| 2 | 4-9 | 7.5-6.5 | 0.8-0.2 | 1.0-0.8 | Normalna | 0.4 | 0.8-1.0 |
| 3 | > 9 | 6.5-5.8 | 0.2-0.1 | 0.4-0.8 | Lekko zmętniała | 0.25 | 1.2-1.5 |
| 4 | Nie można zmierzyć | <5.8 | <0.1 | 0.2-0.4 | Silnie zmętniała | <0.2 | >1.5 |
Correcting keratoconus
orrection with glasses
It is used in the initial stages of the cone development , where the astigmatism is not large and regular enough . It is also effective when the cone is located far away from the optical center.
Further development of the disease necessitates contact lenses or surgical procedures.
Soft lenses Correction with toric soft lenses – theoretically possible, but for the high susceptibility and the tendency to surface projection of irregularities, this method usually does not produce satisfactory results.
Correction with hybrid lenses and duo systems
In case of highly irregular corneas in over- sensitive to the presence of a foreign body in the eye or in the case of “weak” corneal epithelium, recurrent erosions, hybrid lens can be selected or so-called . duo-systems (two corrective hard lenses and soft carrier – protective).
This solution is seemingly ideal, as it combines the convenience of carrying and good optical correction, but often leads to a decrease of mobility of the lens and dangerous cornea hypoxia leading to vascular neoplasia within cornea. This problem is even greater as it applies to people who are expected to undergo penetrating kerato-plastics . For these reasons, the solution should be a last resort. Slightly fewer risks have duo -systems applied temporarily only when we observe periodic intolerance to hard lens.

Photo. 5. Vessels entering deeply into cornea
Correction with hard lenses is the most popular. Full range of spherical lenses , aspherical -curve , specially designed for the correction of the cone are applied . Initially flat lens were fitted so as to squeeze the cone summit . Today there are alternatives in the form of ClearKone hybryd lenses , which have a rigid part that protects the corneal epithelium , but due to the soft part of the lens and tendency to suction , they have limited application .
Fitting without touching the top of the cone , which is used for maximum protection of the cone , also cannot be widely applied because of the minimal improvement in visual acuity and too little mobility of the lens with a tendency to aggregate within the top of product metabolism taking place during hypoxia ( hypoxia ) . That additionally worsens the condition of the already affected cornea.
Contour three-point fitting is now the most recommended ,maximally parallel to keratoconus . It requires the use of a variety of lenses from different manufacturers, often individually modified for a given case. It is very desirable to use of topography of the cornea, which not only speeds up the application of lenses, but allows to select the most suitable geometry of the contact lens .
Surgical correction
- Petrating keratoplasty is a procedure, in which degenerated by disease tissue is replaced by healthy tissue given by a donor.
- Cross-linking,
- INTAXES,
- Cornea transplants